341 Racetrack Road NW Fort Walton Beach, FL 32547
120 E. Redstone Ave. Suite A Crestview, FL 32539
Call Us Today
-
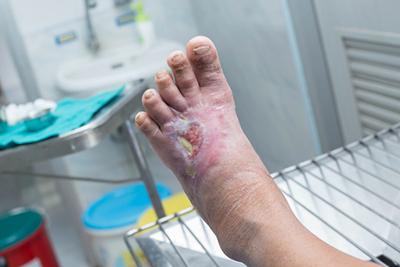
Diabetic Foot Care: Managing Risk and Preventing Complications
posted: Mar. 19, 2024.

-
Managing Foot Pain: When to See a Podiatrist
posted: Mar. 17, 2024.

-
The Basics of Podiatry: What Does a Podiatrist Do?
posted: Mar. 15, 2024.
-
Understanding Arch Pain: Causes and Common Conditions
posted: Feb. 08, 2024.

-
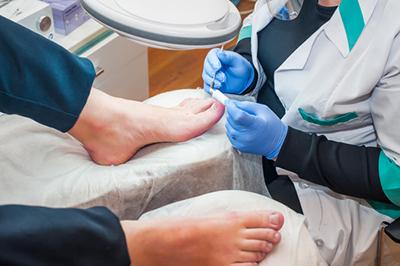
Surgical Interventions for Diabetic Foot Wounds: Procedures and Recovery
posted: Feb. 05, 2024.
-
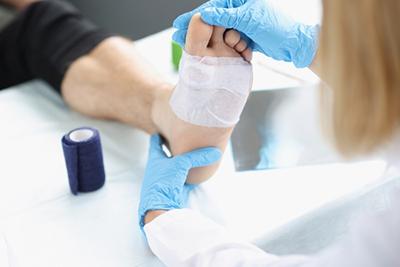
Understanding Common Foot Conditions: A Comprehensive Guide by Your Podiatrist
posted: Jan. 26, 2024.
-
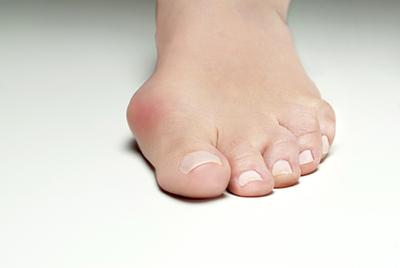
Diabetes and Foot Care: Tips for Maintaining Healthy Feet
posted: Jan. 16, 2024.

-
Understanding Plantar Fasciitis: Causes, Symptoms, and Treatment
posted: Dec. 22, 2023.
-
Running and Achilles Tendinitis
posted: Dec. 08, 2023.

-
How Your Podiatrist Can Relieve Your Arch Pain
posted: Nov. 21, 2023.
-
How Nail Fungus Treatment Can Suppress Infections
posted: Nov. 08, 2023.
-
How Your Podiatrist Can Relieve Your Arch Pain
posted: Nov. 06, 2023.
-
Plantar Fasciitis: A Comprehensive Guide to Understanding and Managing Heel Pain
posted: Oct. 11, 2023.

-
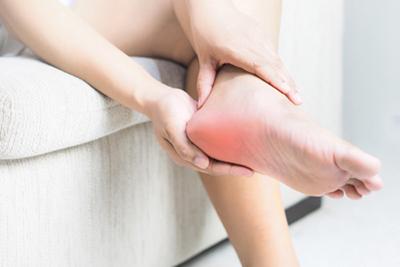
Frequent Causes of Heel Pain
posted: Sep. 25, 2023.
-
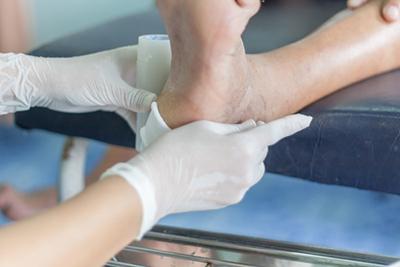
How to Care for Diabetic Wounds
posted: Sep. 05, 2023.
-
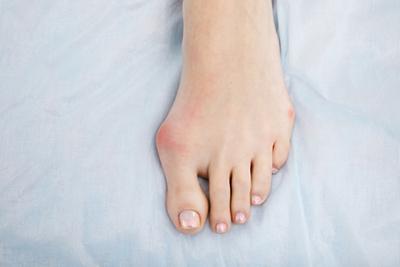
Common Foot Problems
posted: Aug. 21, 2023.
Contact Us
Send Us an Email
Crestview Office
Fort Walton Beach Office
Hours of Operation
Monday:
8:30 am-5:00 pm
Tuesday:
8:30 am-5:00 pm
Wednesday:
8:30 am-4:00 pm
Thursday:
8:30 am-5:00 pm
Friday:
8:30 am-4:00 pm
Saturday:
Closed
Sunday:
Closed